Ripal H. Patel, MD, MPH, shares his thoughts on what it was like getting COVID-19 and why he is a supporter of the vaccine.
They say doctors don’t get sick. Call it machismo, call it pride, or call it a steadfast devotion to our patients, who we feel need us to stand strong as we commit ourselves to treating their illness.
So when, during the early months of the pandemic in April, I came back to my house and began to feel dizzy, lightheaded, and warm, I knew something was wrong. I rushed up to my bedroom, grabbed the temperature gun, and aimed it at my forehead. I heard a beep, then saw a dark, red flash. 102.4. That image will forever be with me.
Despite all my attempts to stay safe, I had succumbed to COVID.
Getting infected
I’m fairly confident I know how I got infected. One day during the onset of the pandemic, as we were all adjusting to wearing suffocating amounts of PPE seeing patients and becoming more adept in their triage, I stepped out to retrieve lunch for my residents.
As I walked out of the ER to the waiting room, I let my guard down just once. I was adjusting to the N95s and shields and needed some fresh air. As I went to meet the delivery person, I saw my technician Juan on the ground in a panic holding an elderly patient that was seizing and vomiting. Juan had frantically turned him to his side, and I rushed over to assist. Time was crucial as the patient was at risk for aspiration, a condition when the contents of your stomach go into your lungs. I was fairly close to his mouth as particles spewed out, not realizing later that I forgot to pull up my mask. As we brought him back to our resuscitation area, I found out later he was COVID+. I became symptomatic 3 days later.
Sick and isolated
People often ask me what it was like. My response: horrific, and lonely. Simply horrific, and lonely. I’ve never been so sick in my entire life.
It started with fevers not entirely responsive to Tylenol or Motrin. They went as high as 104. My head felt like I was in a constant sauna, a steamy fog where the temperature wouldn’t go down, and I couldn’t escape. This was coupled with crushing body aches, retching, and loss of appetite. I could feel myself losing weight (8 pounds in total), and yet I had no desire to eat. My stomach was a tight knot. As I lay in bed, I slept almost 18 hours a day. Darkness begot darkness. I had to utilize all 4 regions of my bed, because I soaked through the sheets with sweat. As one puddle was formed, I summoned the faint energy I had to shift to another portion of the bed, shedding off clothes to try to cool down. At a certain point, I was too weak to stand, and with the sheets soaked in sweat, I rolled off the bed with a thud and blacked out on the floor. Lying there in boxers, pouring in sweat, weak but no desire to eat, and a headache so severe I felt like my skull was being pressed on and my brain would burst out from my ears. And all the while, too weak to even pick up my phone and dial my family.
Experience leads to understanding
That was probably the absolute low point. And yet, the only beacon of optimism I saw from this was something an old attending once told me in medical school: How will you understand what your patients are experiencing if you haven’t experienced it yourself?
I think back to one of the sickest COVID patients I had during the summer. It was an 85-year-old Indian man, with several medical problems like high blood pressure and diabetes. I was actually called in to assist another physician, because he only spoke one of my native tongues, Gujarathi. He was gasping for air on a BiPAP machine, with a piercing look of terror, of fear, and of suffering, that bore through me. I was paralyzed and was fumbling trying to speak my broken Gujarathi to him, explaining that he may need intubation.
The patient was in such a state of shock he was desperately scrambling in all directions thinking some position — some way to comfort his body and lungs — would help him breath better. It was like someone clawing through water to reach the surface deep in the ocean but being weighed down to drown. We called his son in New York. Through the shouting, piercing alarms declaring his low oxygen levels, the son was begging him to please take the tube. That horror in his eyes, that ominous sense, for once I could empathize, as I had laid there in my bedroom many months ago.
Waiting for a vaccine
I prayed for the vaccine like many. Each time I watched the news, it seemed as though that was incessantly the question. COVID is deadly yes, but beyond deadly, the world quickly realized the healthcare systems were simply not at capacity to handle the onslaught of patients that required emergent care. We all expect if we get sick, we go to the ER, we see a physician in a somewhat timely manner, and a bed will be available including the resources, medications, and nurses. Now imagine a world where that expectation — that faith you place in the system — is gone. That is exactly the world the novel coronavirus created.
And so I got the vaccine, and frankly, I had no hesitation about taking it. Why? The science was sound, the trials large and well-conducted, and — as if the pharmaceutical companies knew the potential hesitation — designed it as an mRNA vaccine, so that no actual active or dead virus would enter our bodies.
Many asked me about side effects, and I was quick to remind them we have been vaccinating for decades, often with vaccines in a three part series, and thus most major side effects occur within 6 weeks, for which these trials had addressed. I also explained to them the Chinese had shared the genetic sequence with the world early in the pandemic, and this was then in tandem with fierce global competition coupled with the FDA obliterating bureaucratic red tape for approval.
And so, like watching food delivered to our doorsteps with an app or having a video chat with my relatives in India from the U.S. anytime of day for free, the vaccine itself stands as another true technological achievement that is simply humbling.
In support of vaccination
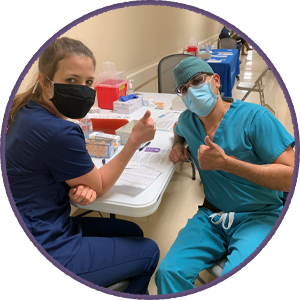
So, as I got my jab, I became one of many on social media supporting the movement. We have a solution, and only when people feel safe, when we feel the pandemic is controlled, will we be able to move towards that not-so-elusive goal of getting things back to normal, before COVID-19 took the world down.
I am not much for politics. Nor am I religious. But, all my life, I have always held science in due reverence. Perhaps an homage to Carl Sagan. Hypothesis, experiments, and robust data to support a notion. When I think of my parents, I have to know that if there was a way for me to protect them in case they were infected — and if I didn’t seize it — I couldn’t live with myself.
And so, as the vaccine rolls out to healthcare workers and the elderly, and eventually to the population at large, I don’t demand you take it. All I ask is to get educated, to speak to physicians and healthcare professionals, to read about the studies from non-biased sources, and ultimately, I am confident the world will make the sound decision.


